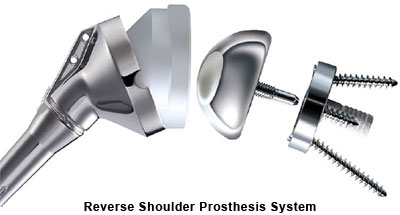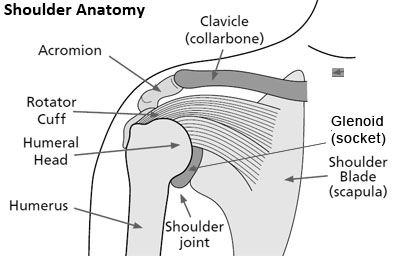
The shoulder is a ball and socket joint, made up of three bones, the humerus (upper arm bone), the scapula (shoulder blade) and the clavicle (collar bone). The ball at the top end of the humerus (humeral head) fits into the socket (glenoid) of the scapula to form the shoulder joint. The humeral head and glenoid are covered with cartilage, which allows for smooth joint motion.
The shoulder has the greatest range of motion of any joint in the body, allowing you to position your hand anywhere in space. The coordinated activity of numerous muscles working together in set patterns is required to produce this motion.
The rotator cuff is a group of muscles closely wrapped around the top of your arm bone (humerus). These muscles originate from your shoulder blade and their tendons form a cuff which covers the joint. The rotator cuff muscles are important to normal shoulder function. Together they act to stabilize and rotate the shoulder joint.
In the Arthritic shoulder the normal cartilage (smooth surface of joint) is worn away and there is bone-on-bone without the normal smooth gliding surfaces, which are able to glide on one another with little friction and wear. The joint may also become irregular from boney growth (osteophytes), which is the body's attempt to "heal" the cartilage injury.
Pain is usually due to the irregular joint surfaces rubbing on one another and from the inflammation of this wear and tear. If you can't lift your arm, perform everyday tasks or sleep at night, your doctor may recommend arthroplasty, the medical name for a shoulder replacement operation.
The surgeon removes the damaged parts of the shoulder and replaces them with artificial parts. The surgeon can replace either just the head of the humerus bone, the ball, or replace both the ball and the socket, the glenoid.
An incision is made in the front of the shoulder, and the humeral head (the ball) is removed. The new ball and stem are then inserted into the bone. If the surgeon is carrying out a total shoulder replacement, the socket side of the joint is then smoothed and the new plastic socket is attached securely in place.
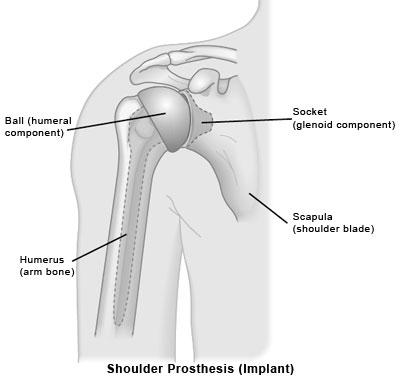
If the humeral head (the ball) is severely fractured but the socket is normal, with healthy and intact cartilage, your surgeon may recommend replacing only the ball. This procedure is called hemiarthroplasty. Sometimes, surgeons make the decision between a total shoulder replacement and a hemiarthroplasty in the operating room at the time of the surgery. Studies have shown that patients with osteoarthritis get better pain relief from total shoulder replacement than from hemiarthroplasty.
Shoulder replacement materials are technologically advanced, and are identical to the materials used in knee and hip replacements. The ball and stem are made from titanium and cobalt chrome metals; the socket is made of plastic called polythene.
For a brief demo of the procedure, visit Total Shoulder Replacement
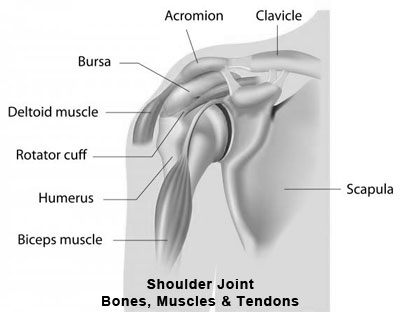
A standard total shoulder replacement depends upon muscles and tendons around the shoulder joint to be intact. These muscles and their tendons function to move the shoulder and are together called the rotator cuff. When these tendons become extensively torn so that they do not attach to the bone any longer, the shoulder often does not function normally. The loss of the rotator cuff can produce pain and also loss of motion. A normal shoulder replacement is designed to work only if those tendons are intact.
Reverse Shoulder Replacement (Arthroplasty) has emerged as a very attractive alternative for patients with cuff-tear arthropathy, selected proximal humerus fractures and nonunions. Its indications continue to expand, especially for revision surgery.
Without an intact rotator cuff, the ball can ride high in the socket and wear abnormally, creating abnormal contact forces across the joint. Over time this leads to 'cuff-tear arthropathy.' In the later stages of a cuff tear, the patient develops arthritis in the shoulder and the result is constant pain, weakness and lack of function. The pain is so severe that patients suffering from cuff-tear can't sleep at night; they can't do their activities of daily living. They get depressed about their shoulder and it's affecting everything about what they do and who they are.
Reverse or Inverse Total Shoulder Arthroplasty (RTSA) is designed specifically for the treatment of glenohumeral (GH) arthritis when it is associated with irreparable rotator cuff damage, complex fractures as well as for a revision of a previously failed conventional Total Shoulder Arthroplasty (TSA) in which the rotator cuff tendons are deficient.
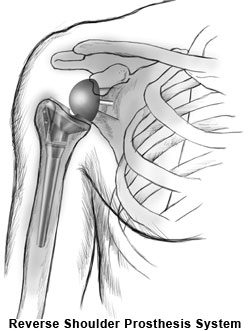
Like standard shoulder replacement surgeries, the arthritic joint surfaces are replaced with a highly polished metal ball attached to a plastic socket. But in the reverse procedure, the socket and metal ball are switched. The reverse procedure constrains the ball in a cup that is inserted into the end of the humerus and the metal ball is attached to the shoulder bone. This allows the patient to use the healthier, stronger deltoid muscle instead of the torn rotator cuff to lift the arm.
Anyone who has a condition that predisposes them to an infection is a poor candidate for RTSA. That may include patients with diabetes, someone who is on an immunosuppressant, or someone with rheumatoid arthritis. And because of the need to affix the prosthesis to the shoulder, patients with poor bone quality are also poor candidates.
The prosthesis system used for Reverse Shoulder Replacement are the opposite of the system used in standard shoulder replacement. In this socket and metal ball are switched as shown in the image below.